 The Union and state governments must evolve a comprehensive, evidence-based mechanism to bring in private health services in a systematic and coordinated care model
The Union and state governments must evolve a comprehensive, evidence-based mechanism to bring in private health services in a systematic and coordinated care model The Union and state governments must evolve a comprehensive, evidence-based mechanism to bring in private health services in a systematic and coordinated care model
The Union and state governments must evolve a comprehensive, evidence-based mechanism to bring in private health services in a systematic and coordinated care modelThe global crisis, in the wake of the COVID-19 pandemic, has underscored the indispensability of a strong public healthcare system. As is the case with many other countries, in India too, the crisis exposed the weakness of the health system.
Due to systemic challenges that have perennially crippled the government health system, the response has been grossly inadequate. But the public sector and particularly the brave frontline health workers have been the only respite for people.
However, the role of private sector has been inadequate in overcoming the national crisis. Several news reports have exposed the regressive nature of the private sector. Either patients are being denied care, or charged high fees or being subjected to unnecessary tests to make money. There are also reports that patients' families are being beaten up for non-payment.
Here we would like to discuss some key features of private health care delivery in India, with an attempt to demystify some conceptions related to private health care delivery and point out some key concerns.
Also Read: Coronavirus pandemic leaves private healthcare sector in financial distress
We would primarily use the two latest NSSO rounds Household Social Consumption: Health, the 71st (2014)[i], and 75th rounds (2017-18) and complement them with some other data sources.
Myth one: Private sector delivers care where government does not reach
The National Health Policy 2017 recognised private sector as an engine of growth. Several other policy pronouncements have been made with the understanding that the private sector complements government health services. Although the sector has grown significantly in the last three decades as an outcome of a series of reforms, much of this growth took place in metropolitan cities.
The government funded health insurance (GFHI) schemes, like the Prime Minister's Jan Arogya Yojana (PMJAY), are fuelling further expansion of for-profit private hospitals through transfer of public resources to ensure a reasonable market in smaller towns.
At the outset, the plurality of the private health sector must be emphasised upon. The private sector is not a homogenous entity. It has both formal and informal providers as well as for profit and not for-profit entities under it.
The non-corporate private sector comprises of single doctor dispensaries, 2-10 bed nursing homes, medium-sized facilities. Additionally, India has the facilities of the recognised traditional systems of medicine. Meanwhile, the formal sector comprises large corporate hospitals, diagnostics chains, and stand-alone super specialty facilities.
There is hardly any comprehensive data available on the size and composition of the private sector. However, a census of health facilities in 63 major cities conducted in 2012 suggests that the distribution of private facilities favours metropolitan cities.
Distribution is most skewed in case of corporate hospitals as around 67 per cent of them are located in big cities. Some of the notable big cities include the four metros--Mumbai, Kolkata, Delhi, Chennai, and upcoming metros such as Ahmedabad, Bangalore and Pune.
Mumbai has shown the highest presence of health facilities among all the big cities. Out of 13,413 private facilities across all cities, Mumbai alone has 2,119 facilities - contributing to around 16 per cent.
As per the Periodic Labour Force survey (2017-18) data, out of every seven doctors only one is located in rural areas, rest of the six are located in urban areas.
In the context of COVID-19, a key requirement for critical cases is the ICU beds. Approximately there were around 49 thousand ICU beds in private sector across all the cities. However, half of these beds are in 10 major cities, where the shortage of tertiary care facilities are less acute as many government medical colleges are located in these cities.
As per the 2012 data, there were more than 27 thousand ICU beds in public sector in these top ten cities. Thus, the private sector, rather than complementing the services of government, mushrooms around the tertiary government institutions to draw from the health care ecosystem created by public investment.
Another key feature of private hospitals is that most private facilities have less than 10 beds in their ICUs, which makes these places unviable for effective management of critical cases. Majority of the private sector outside these metro cities is much smaller in size, often equipped with five or less ICU beds. Rather than complementing public institutions, the private sector mushrooms around big government institutions.
Myth two: Private sector delivers 80% of care
Any discussion on health care delivery in the country starts with this emphatic assertion that private sector delivers 80% of care in the country. Though it is partially true that the majority of health care is delivered in the private sector, there are certain important trends to be noted.
First, private provisioning is more in case of out-patient (OP) care, however in the last 15 years, there has been a continuous decline in the utilisation of private care for OP care. Out of every 100 outpatient visits in rural areas, more than 67 took place in various types of private-both for-profit and not-for-profit facilities during 2017-18.
However, this is a decline from 72 in 2014 and from 78 in 2004, meaning that over the years an increasing proportion of people are moving away from private facilities. In urban areas, the overall utilisation of private facilities is more compared to rural areas, but there seems to be a gradual decline since 2004.
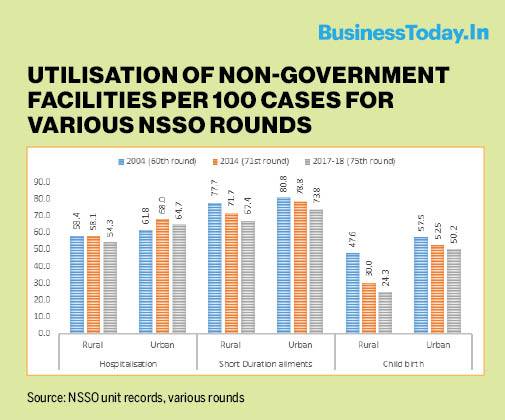
The use of private facilities is less for hospitalisation care compared to OP care. Out of every 100 hospitalisation cases, 54 and 65 are treated in private hospitals in rural areas and urban areas respectively.
In rural areas, the utilisation of private facilities has declined since 2004. In 2014 out of every 100 hospitalisation cases, 58 were treated in private hospitals. In 2017-18, this has declined to 54. Though the utilisation of private facilities is more common in urban areas, there was some decline between 2014 and 2017-18.
Reliance on private sector for child birth has also declined since 2004. The most significant decline is in the rural areas.
During 2004, almost half (47.6%) of the institutional deliveries were happening in the private sector. Thanks to initiatives like the National Rural Health Mission to promote institutional delivery and strengthen services in public facilities around child birth, now more than three-fourth of the institutional deliveries in rural areas happen in public facilities. In urban areas too, there has been a decline in private sector utilisation for child birth.
The utilisation of facilities varies considerably by economic class. With increasing well-being (measured in terms of consumption expenditure), people tend to utilise private facilities more and less of government facilities. In the bottom three quintiles, half or more people go to public facilities in rural areas. In urban areas, even among the poorest groups, more than half of the hospitalisation cases are treated in private facilities.

Apart from inadequate expansion of public sector hospitals and complaints about poor service quality (which is not the same as clinical quality), there has been a continuous push towards the private sector through the plethora of GFHI schemes, the latest Avatar being the PMJAY.
All of this together creates a situation where people, even from the economically vulnerable groups, are left with no other choice but to access private institutions.
Myth Three: Private care is free with insurance
A lot of people get drawn towards private sector and health insurance schemes because of the promise of free care. Free care through insurance is another major myth.
Apart from GFHIs, there are other insurance schemes that are sometimes organised by employers on behalf of their employees.
Then there is private voluntary health insurance (PVHI) that households buy for themselves.
Also Read: Coronavirus Lockdown XI: Why India's health policy needs a course correction
COVID-19 experience has shown that there is very little that private sector can offer in terms of reducing costs of care. Let us first start with how much households were paying on average for each hospitalisation episode in 2017-18 compared to 2014.
In order to do this effectively, we need to adjust the average expenditure of 2017-18, taking out the effect of rise in prices between the two periods.
Out-of-pocket expenditure (OOPE) for hospitalisation has declined during this time period in terms of constant prices. The decline is steeper in urban areas compared to rural areas, though costs are generally higher in urban areas.
How much households would have to pay would depend on whether they choose to go to public or private hospitals for similar care needs. Public sector costs have decreased considerably in both urban and rural areas. Private sector costs on the other hand have increased in rural areas while declining marginally in urban areas in real terms, while it has increased in nominal terms.
In urban areas, people had to pay 3.6 times more in private sector compared to public hospitals in 2014. In rural areas this ratio is 3.3 times. In 2017-18, cost ratios increased to 5.8 and 5 for urban and rural areas respectively. Thus private sector costs are increasing rapidly while the public sector has been able to reduce the burden on households to some extent.

It is understandable that household costs in private sector would be higher compared to public hospitals. In public hospitals care is heavily subsidised, whereas in private sector, unless one has insurance coverage, the costs and profits are recovered basically digging into peoples' pockets.
Then is it the case that people with insurance coverage pay less compared to others? Clearly there is heavy expenditure incurred by households even if they have access to insurance and end up going to the private sector.

Policymakers at the National Health Authority and the NITI Aayog, who have so far been very vocal about handing over health care delivery to the private sector, have acknowledged in a recent press statement that PMJAY utilisation has gone down drastically during the lockdown phase.
As per the NHA report, between February and April, the number of treatments for essential non-covid procedures by both private and government hospitals across the country dropped by more than 20 per cent, mostly due to the coronavirus-induced lockdown.
During this two-month period, the number of procedures performed in those packages dropped to 1,51,672 from 1,93,679, the report said further. Between February and April, cancer-related procedures fell by about 57 per cent; cardiology by 76 per cent, and procedures in obstetrics and gynaecology fell by nearly 26 per cent, the report added.
As per news reports, the hospital bill for a COVID-19 patient with a five-day stay along with ICU facility usually crosses Rs 5 lakh. As per the latest PLFS data, only 5% population has an annual income of more than Rs 5 lakh. Therefore, either the vast majority would not be able to afford these rates, or resort to selling assets or borrowing.
Out of every three rupees spent on health, two rupees come from peoples' pockets in our country. Four out of ten rupees spent from pocket is on account of hospitalisation. High health care costs cause financial hardship for households, push them below poverty, and force them to borrow or sell assets.
Around 10.6 crore people are impoverished because they had to pay out of pocket for hospitalisation in 2017-18. Of these there are 6.8 crore people who live in rural areas. In the current context, while every household of the country is facing hardship and crores of people have been impoverished due to lockdown, the situation would be worse.
Thus the private sector neither complements the care provided by public sector, nor is it the dominant provider beyond OP care; nor could the claims of free care be substantiated.
On the other hand, with relatively less amount of investment, the public sector provides a significant part of clinical care along with an entire range of preventive care and public health services. At the same time, dependence on private sector is essentially iniquitous and impoverishing.
Myth four: private sector is efficient and it just needs regulation
It has been observed historically that for-profit private hospitals fail to ensure mechanisms that can provide effective treatment in case of public health emergencies.
There are certain typical market failures that define the functioning of private sector. Creme skimming, where more critical cases are refused and relatively safe patients are admitted, is quite common. Induced demand where information asymmetry is used to induce unnecessary care to patients and thereby charging high fees is another way through which the private sector makes money.
In times of public health emergencies, these tendencies become more prominent as people are more desperate and thus bring out more severe consequences on their lives. At this juncture any engagement with the private sector should strictly be in non-commercial terms where ensuring free care to patients and strict adherence to treatment protocols becomes key.
Waking up to the plight of people and denial of care, the Supreme Court and some state governments have attempted to cap the COVID-19 treatment prices. However, there are problems with partial price regulation.
The experience of capping stent prices suggests that the private sector would switch the burden to other charges and reap profit. The same is likely to happen in case of COVID-19 treatment. There is a need for comprehensive price regulation for all kinds of services.
If care can be delivered at regulated prices through PMJAY, CGHS or other insurance package rates, there is no reason similar care cannot be delivered at similar costs to individuals who do not have any protection of insurance.
The very first step towards this would be full disclosure of costs and prices under the Clinical Establishment Act and that a health care price index is developed which is sensitive to location and type of facility for the types of care provided. Such an effort would also help in better pricing of insurance packages.
The Union and state governments must evolve a comprehensive, evidence-based mechanism to bring in private health services in a systematic and coordinated care model. Any attempt to bring private sector hospitals into the net of publicly provided care should be on the basis of needs, competence and complementarity, rather than ad hoc arrangements.
Closing observations
To overcome the current challenges faced by the health system, a lot needs to change. First and foremost would be to build a strong pro-people non-commercialised public system as an alternative to the dominant for-profit sector.
This is the only way rational and good quality care can be delivered to the majority of the people. A strong public sector also works as the most effective means to regulate prices and practices in the private sector.
However, none of this can be achieved if we do not invest adequately in health. The current public spending of 1.15% of GDP on health is clearly suboptimal.
Unless we increase public investment in health to at least three per cent of GDP in the medium term and strengthen the government health system starting from primary care, peoples' miseries would continue and healthcare will continue to result in hardship and unbridled profit simultaneously.
(Indranil is an Associate Professor, OP Jindal Global University, and Montu Bose is an Assistant Professor, TERI School of Advanced Studies.)